If you have ADHD and you've cycled through three medication trackers in the last year, you're not bad at apps. The apps are bad at ADHD. The standard medication app design assumes you can hold a multi-step setup in working memory, respond to notifications on the first try, and maintain interest in a tool that looks the same every day. Those assumptions break down fast when executive function is the thing that's impaired.
We wrote about why ADHD makes you forget your meds - the neuroscience behind it. This piece is about the other half of the problem: why the tools designed to help often make things worse, and what ADHD-friendly design actually looks like.
Why do most medication apps fail people with ADHD?
Most medication apps fail people with ADHD because they demand the cognitive skills the condition impairs. Working memory, task initiation, sustained attention, and time awareness are all executive functions - and all are disrupted by ADHD. When an app requires four steps between "open" and "done," each step is a point where the ADHD brain can exit.
The numbers confirm this. A clinical trial of the Inflow ADHD app found that 54% of participants dropped out within seven weeks. Most left before the two-week mark (PLOS Digital Health, 2022). Across mental health apps more broadly, average 30-day retention sits around 4.2% (JMIR, 2024). For ADHD users, that number is likely worse.
Russell Barkley, one of the leading researchers on ADHD and executive function, frames ADHD as a disorder of self-regulation rather than attention (Journal of Developmental & Behavioral Pediatrics, 1997). The popular understanding of ADHD as "can't focus" misses the point. People with ADHD can focus with frightening intensity during hyperfocus. What they struggle with is directing attention on demand, holding instructions in working memory, and bridging the gap between intention and action.
An app that requires you to navigate three screens to log a dose is asking you to hold that intention across each screen transition. For someone whose working memory clears between rooms - let alone between screens - that's not a minor ask. It's a design failure.
When the tool demands the same abilities the condition disrupts, the result isn't productivity. It's frustration, guilt, and another abandoned app.
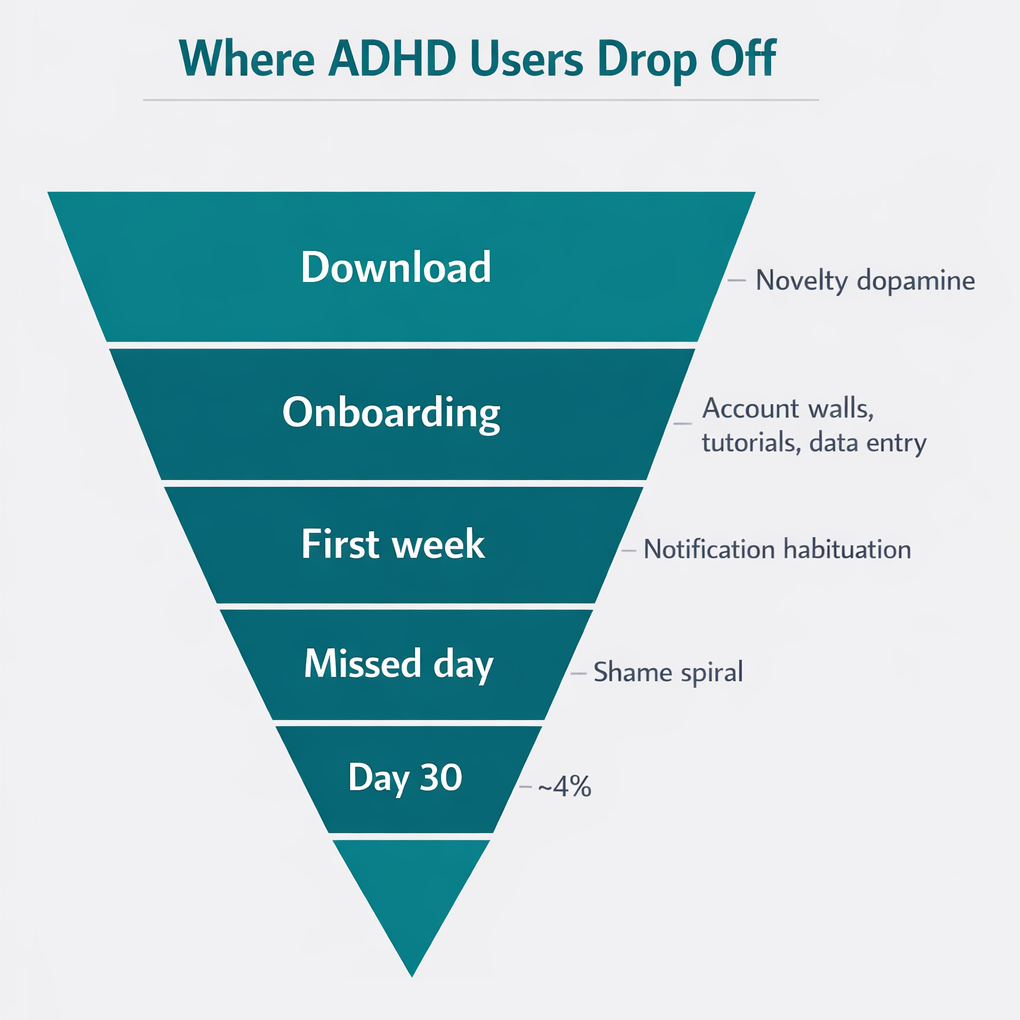
What makes onboarding so hard for ADHD brains?
The gap between downloading an app and using it successfully is where most ADHD users fall off. Researchers call this the "onboarding cliff" - a steep drop in engagement that happens in the first few sessions, before the app has had any chance to prove its value.
Every screen that stands between "install" and "working" is a cognitive tax. Account creation forms ask for email, password, name, date of birth. Setup wizards want medication names, dosages, schedules, refill dates. Some apps force a tutorial you can't skip. Each of these steps burns executive function that ADHD brains don't have in surplus.
People in ADHD communities describe what they call "The ADHD App Cycle": download a new app, hyperfocus on setting it up for a few days, then forget it exists because it became part of the background. The initial novelty provides enough dopamine to power through setup. Once that wears off, the app needs to justify itself on every single open. If daily use takes more than a few seconds, it won't survive.
One Reddit user who built a productivity timer for his wife with ADHD described the design goal: "Open app. Press start. Done. No account. No onboarding. No tutorial." His wife had been "overwhelmed by options and dashboards" in other tools. Three screens of setup was three screens too many.
The practical implication is clear. Any medication tracker that requires an account before you can set a reminder is filtering out a large portion of ADHD users at the door. The app isn't collecting information for your benefit - it's collecting data. And ADHD brains, already carrying the weight of Schedule II medication stigma, have good reason to resist handing over personal details before they even know if the app works.
When do streaks become shame spirals?
Streaks become shame spirals when a missed day triggers Rejection Sensitive Dysphoria - an intense emotional response to perceived failure that's common in ADHD. The broken streak becomes a visible record of failure, triggering self-blame, avoidance, and often permanent app abandonment. Binary pass/fail tracking conflicts directly with ADHD neurology.
RSD is an intense emotional response to perceived failure or criticism. It's not an official diagnosis, but clinicians like Dr. William Dodson have documented it extensively in ADHD populations. Experts estimate that children with ADHD receive roughly 20,000 more corrective or negative messages than their neurotypical peers before age twelve (ADDitude Magazine). By adulthood, many people with ADHD have a deeply wired sensitivity to anything that looks like failure.
A streak counter exploits this vulnerability. Maintaining a 30-day streak feels motivating - until day 31 breaks. For a neurotypical user, that's mild disappointment and a fresh start. For someone with ADHD and RSD, the broken streak becomes what Dodson calls a "monument to failure." The app that was supposed to help now represents another thing they couldn't stick with. Many users never open it again.
The pattern has a name: the shame spiral. A missed day triggers self-blame. Self-blame triggers avoidance. Avoidance means more missed days, which compounds the shame. The app's streak counter ticks down or resets to zero, making the failure visible and permanent (Inflow).
There's a second problem with streaks that goes beyond RSD. ADHD brains run on interest-based motivation, not importance-based motivation. A neurotypical brain can push through a boring task because "it matters." An ADHD brain needs the task to be novel, urgent, or personally interesting. Streak counters provide novelty for the first week or two. Then hedonic adaptation kicks in - the dopamine hit from maintaining the streak fades as the brain adjusts. For ADHD brains, which already struggle with reward sensitivity, this fade hits harder and faster.
What works instead of streaks
Apps designed with ADHD in mind use different patterns:
- Flexible intensity scales (0-5 instead of binary yes/no) so a partial day still counts
- Forgiving streaks that don't reset to zero on a missed day
- Variable rewards - surprise badges or unlockable content rather than predictable points
- Supportive language when doses are missed ("Carried over to tomorrow" vs. "Streak broken!")
The design principle: an ADHD-friendly app should be, as one UX researcher put it, "fundamentally incapable of causing a shame spiral."
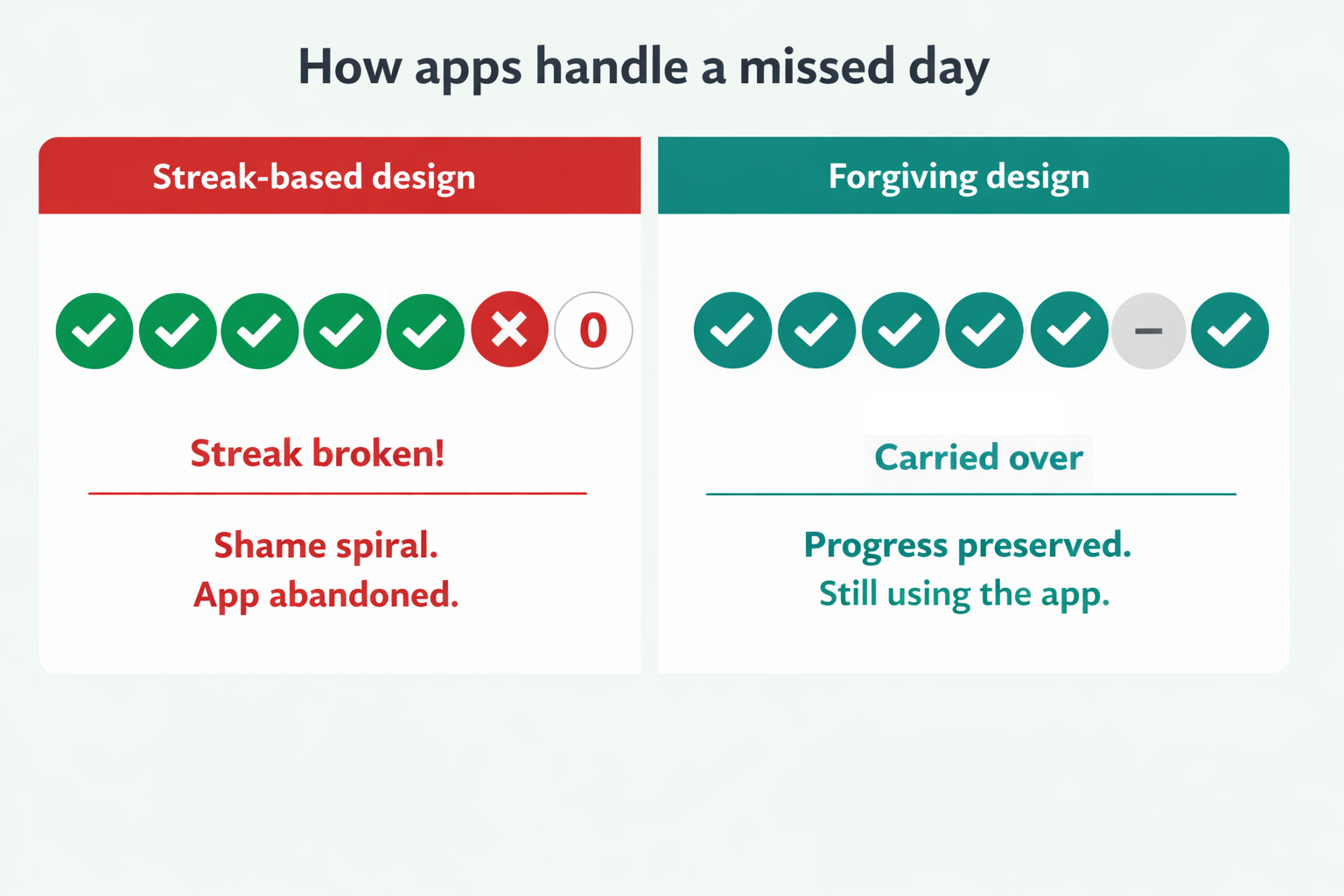
Why do medication reminders stop working?
Medication reminders stop working for ADHD users because the brain adapts to repeated identical stimuli faster than most designers expect. A study on SMS reminders for adults with ADHD found they increased engagement during the second week - but not after. The effect vanished as habituation set in (Frontiers in Digital Health, 2022).
This matches clinical alert research more broadly. A systematic review found that a clinician's likelihood of responding to an alarm dropped by 30% with each additional reminder alert (PMC, 2017). If trained healthcare workers tune out repetitive alerts, expecting ADHD users to respond reliably to the same notification at the same time every day is unrealistic.
There's a specific failure mode that anyone with ADHD will recognize. The notification arrives. You register it. You intend to act. Then something pulls your attention for three seconds and the intention drops out of working memory completely. You don't know you forgot. There's no nagging feeling. The thought was simply deleted.
During hyperfocus, the problem is worse. Alarms fire and get dismissed without conscious registration. The person isn't choosing to ignore the reminder - they're so absorbed that the notification doesn't reach conscious awareness at all.
A counterintuitive finding from adherence research: weekly reminders improved medication adherence more than daily reminders (PMC, 2012). The daily ones became routine and lost their signal. The weekly ones retained novelty. For medication that needs to be taken daily, this suggests the reminder strategy needs to vary - different sounds, different timing, different modalities - rather than firing the same alert on repeat.
A notification you can swipe away is a suggestion, not a reminder. ADHD brains need something that persists until the action is complete.
What does ADHD-friendly app design actually look like?
ADHD-friendly app design reduces friction at every step, forgives inconsistency, and treats the interface as an external support system for executive function - not another demand on it. These patterns align closely with the W3C Cognitive Accessibility (COGA) guidelines, which recommend progressive disclosure, consistent layouts, and task chunking for users with cognitive disabilities.
Zero-friction core actions
The most important interaction in a medication tracker - logging a dose - should take one tap. Not "open app, navigate to medications, find the right one, tap confirm, close modal." One tap. The Theraview ADHD medication tracker gets this right: "tap a prescription and confirm the time." That's it.
Every additional step between "I should log this" and "it's logged" is a point where an ADHD brain can lose the thread. Task initiation is one of the executive functions most impaired in adult ADHD. If starting takes effort, the task won't happen.
Progressive disclosure
Show one thing at a time. Advanced settings, historical charts, refill tracking - hide these behind a second layer. The first screen should answer one question: "Did I take my meds today?" Everything else can wait.
UX designers working on ADHD-specific tools describe this as giving the user "a burst of satisfaction with every click" - each completed micro-step provides enough reward to carry them to the next one (UXPA International). That only works if steps are small enough to feel completable.
External sequencing
Barkley's behavioral inhibition model (Psychological Bulletin, 1997) frames ADHD as a deficit in internal self-regulation. The practical response: externalize the regulation. The app should tell you what to do next, not expect you to remember the sequence. Progress bars, numbered steps, persistent visual cues - these act as what Barkley calls an "external frontal lobe."
If the user needs to add three medications during setup, show "Step 1 of 3" prominently. Let them save after each one and come back later. Don't force the whole sequence in one sitting.
Forgiving mechanics
Inconsistency is a feature of ADHD, not a character flaw. An app that punishes a missed day with a broken streak or a "you missed your dose!" guilt message is fighting the user's neurology.
The apps that survive on ADHD phones handle missed entries quietly. The NoPlex app, designed for ADHD users, sends a simple message when a deadline passes: "The world didn't end; the day just did." DopaLoop uses a 0-5 intensity scale so a partial effort still registers as progress. Neither resets anything to zero.
Clean visual hierarchy
Cluttered interfaces create what researchers call "extraneous cognitive load" - mental effort spent parsing the layout rather than doing the task. For ADHD brains already running low on executive function bandwidth, this extra load can be the difference between using the app and closing it (Medevel).
Effective ADHD-friendly layouts use generous whitespace, limit interactive elements per screen, and make the primary action visually obvious. No walls of text. No competing buttons. One clear thing to do next.
Persistent, varied reminders
A single dismissible notification is designed for brains that convert reminders into actions on the first try. ADHD brains need multiple chances. The best approach combines layered timing (alerts at 15 minutes before, at the time, and 15 minutes after) with varied modalities (sound, then vibration, then a different sound). The reminder doesn't stop until the user confirms the action.
How do you choose a medication tracker that works with ADHD?
Choosing a medication tracker that works with ADHD means looking for design choices, not feature lists. The app with 47 features and a cluttered dashboard will lose to the one that takes five seconds to use every day. Here's what to check before committing.
Can you start without creating an account?
If the app wants your email before you can set a single reminder, it's prioritizing its data collection over your experience. Account walls are the biggest single friction point in onboarding - and for ADHD users, friction is the enemy. A tracker that works without login means you can go from "I just downloaded this" to "my first reminder is set" in under a minute.
How many taps to log a dose?
Count them. Open the app, navigate to the right screen, find the medication, confirm the dose, close the confirmation. If that's more than two taps from opening the app, the daily interaction costs too much executive function. Some apps let you confirm directly from the notification - that's the gold standard.
What happens when you miss a day?
Open the app after a three-day gap and see what it shows you. A wall of "missed" markers in red? A streak counter reset to zero? Or just today's medications, ready to go? How an app handles absence tells you whether it was designed with ADHD in mind.
Where does your data live?
ADHD medications - Adderall, Vyvanse, Ritalin, Concerta - are Schedule II controlled substances. Your tracking data for these medications carries legal and social weight that goes beyond typical health records. If the app stores that data on remote servers, it exists outside your control. A tracker that keeps everything on your device means your medication history stays yours, regardless of what happens to the company behind the app.
We covered this in depth in Where Does Your Medication Data Actually Go? - the short version is that apps that change their pricing or get acquired can take your data with them if it's stored on their servers.
Does it respect your attention?
Some trackers send push notifications for every feature - refill reminders, health tips, weekly reports, social features, upgrade prompts. Each notification competes with the one that matters: "Take your medication." If you can't control exactly which notifications the app sends, it's adding noise to an already noisy system.

The short version
Before committing to a medication tracker, check these:
- Works without creating an account
- Core action (log a dose) takes one or two taps
- Setup takes under five minutes
- No streak punishment or shame-inducing language on missed days
- Reminders persist until you confirm the dose
- Data stays on your device, not their servers
- You control which notifications it sends
If a tracker fails on three or more of these, it wasn't built for how ADHD works - regardless of what the marketing says.
The ADHD app abandonment problem isn't a user problem. It's a design problem with a clear set of solutions. Reduce friction to near zero. Never punish inconsistency. Treat every tap as precious. Keep data local. The apps that get these right don't just retain ADHD users - they work better for everyone. Good design for ADHD is good design, period.
This article is for informational purposes only and does not constitute medical advice. Consult your healthcare provider before making changes to your medication routine.